Bowel Control and Incontinence: Causes, Symptoms, and Pelvic Floor Treatment That Works

Bowel leakage disrupts routine, confidence, and social ease. Many adults experience loss of bowel control at some point, yet few speak about it openly. Research estimates that roughly 8 percent of non-institutionalized adults in the United States report fecal incontinence, with higher rates in older populations. That number reflects real people managing urgency, staining, or accidents in silence.
I write this as a pelvic health physical therapist who treats bowel control problems every week. When someone comes to see me, I focus on restoring control through assessment, retraining, and structured rehabilitation. Education begins that process.
How Bowel Control Works
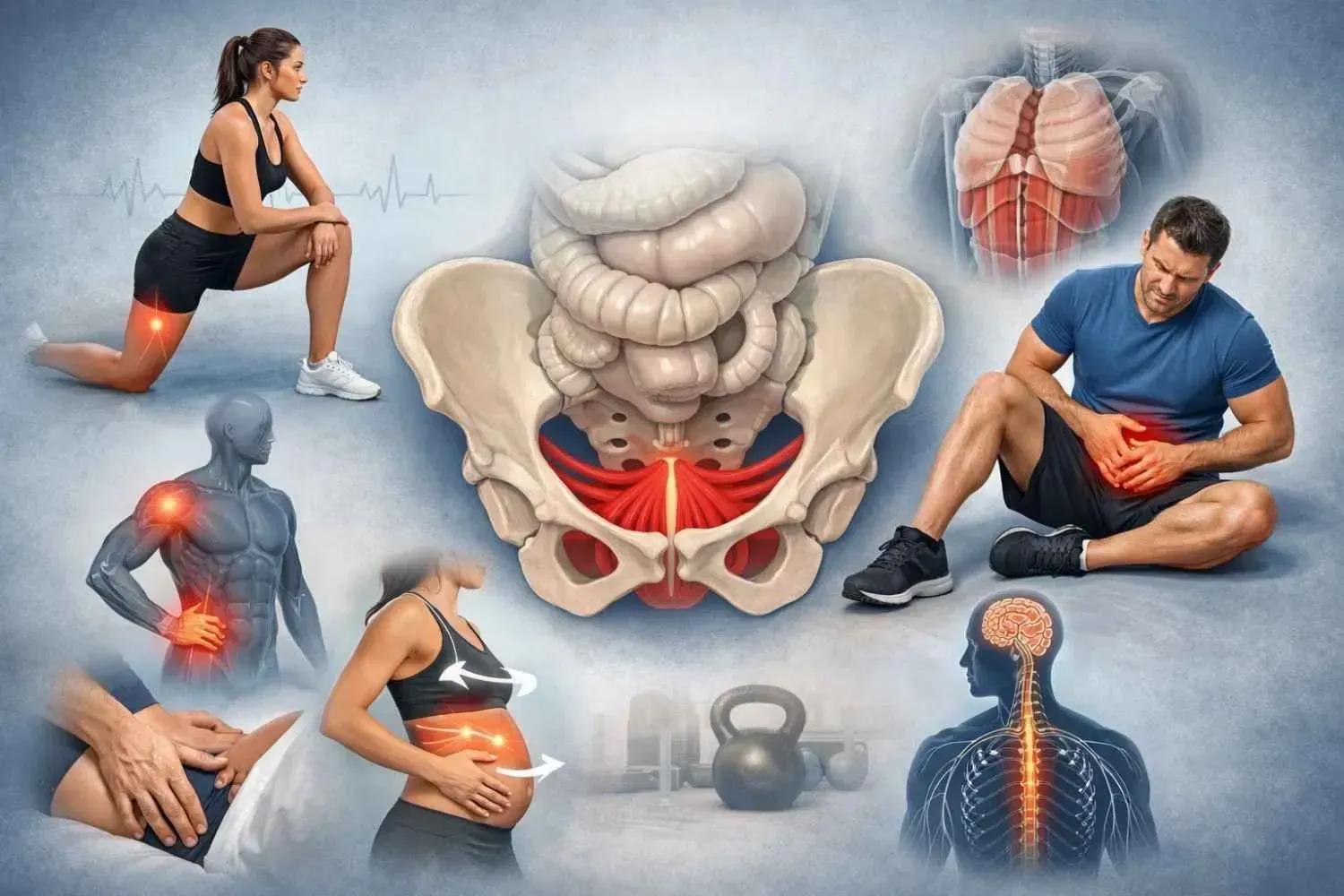
Continence depends on coordination between the rectum, anal sphincters, pelvic floor muscles, and the nervous system.
- The rectum stores stool and senses stretch.
- The internal anal sphincter maintains resting tone without conscious effort.
- External anal sphincter and pelvic floor muscles provide voluntary control.
- Nerves signal fullness and coordinate response.
Rectoanal reflexes allow the body to “sample” contents and distinguish gas from stool. Strong muscles without coordination fail. Intact nerves without muscle strength also fail. Control requires timing, strength, and sensation working together.
When any link weakens or loses coordination, urgency or leakage follows.
Symptoms You Should Not Ignore
People describe bowel control problems in different ways:
- Sudden urgency with little warning
- Leakage during gas passage
- Staining in underwear
- Difficulty holding stool until reaching the bathroom
- Sensation of incomplete emptying
- Bowel accidents during loose stools
Even mild seepage signals dysfunction. Many dismiss symptoms as age-related or temporary. Persistent leakage warrants evaluation.
What are the early signs of bowel control problems?
Early signs include urgency, small leaks, and difficulty delaying bowel movement. These patterns often appear before full loss of control. Early intervention improves outcomes.
What Causes Bowel Incontinence?
Bowel incontinence rarely stems from a single factor. Most cases involve overlapping contributors.
1. Muscle Weakness or Injury
Weak anal sphincter muscles reduce closure pressure. Pelvic floor weakness limits endurance during urgency. Childbirth, pelvic surgery, chronic straining, or aging often contribute.
Postpartum injury deserves attention. Studies show higher rates of anal incontinence in women after obstetric tears or forceps delivery. Many symptoms appear months or years after delivery.
2. Nerve Dysfunction
Nerves carry sensation from the rectum to the brain. Nerve damage reduces awareness of stool arrival or disrupts coordinated contraction. Diabetes, spinal injury, and chronic straining influence nerve function.
Reduced rectal sensation often leads to leakage without warning.
3. Stool Consistency
Loose stool overwhelms control systems. Chronic diarrhea increases urgency and leakage risk. Constipation creates another pattern. Hard stool stretches the rectum, weakens muscles, and causes overflow leakage.
Stool consistency influences continence as much as muscle strength.
4. Aging
Muscle mass declines with age. Nerve conduction slows. Rectal compliance changes. Prevalence rises in older adults, yet age alone does not define outcome. Targeted rehabilitation improves control across age groups.
Is Bowel Incontinence Permanent?
No. Many individuals improve significantly with structured conservative care. Medical guidelines recommend diet optimization, bowel retraining, and pelvic floor rehabilitation as first-line treatment before invasive procedures.
Improvement depends on cause, severity, and adherence to the treatment plan.
Why Generic Kegels Often Fail
People receive advice to “do Kegels.” Many perform them incorrectly or activate surrounding muscles without targeting the anal sphincter. Some individuals over-tighten their pelvic floor, which impairs relaxation and coordination during bowel movement.
Strength without timing does not restore control. Coordination without endurance fails during urgency. Skilled assessment identifies the pattern and corrects it.
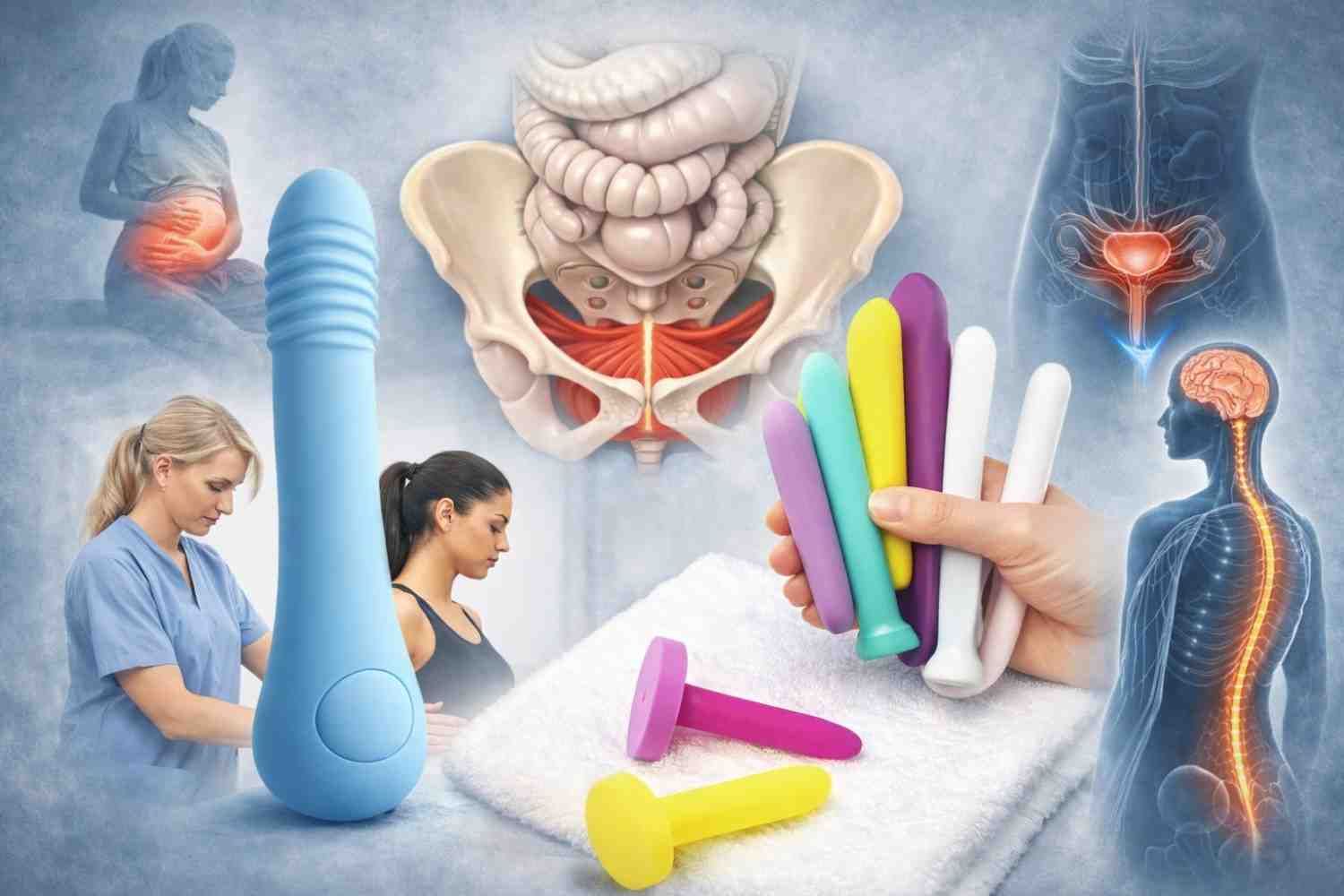
What Pelvic Floor Therapy Actually Does
Pelvic floor therapy addresses mechanics, strength, coordination, and behavior.
I begin with a detailed evaluation:
- Assess anal sphincter strength
- Evaluate pelvic floor coordination.
- Observe breathing and core activation.
- Review bowel habits and stool patterns
- Screen posture and movement
- Dietary assessment
From that assessment, I design individualized rehabilitation.
Strength Training
Targeted contractions improve closure pressure and endurance. Repetition builds the capacity to delay urgency.
Coordination Training
Timed contraction during urge improves control. Relaxation training supports complete emptying without straining.
Bowel Retraining
Scheduled toileting, stool regulation, and urge management restore predictability.
Functional Movement Integration
Breathing patterns, core stability, and posture influence pelvic floor pressure. I retrain movement patterns to reduce strain.
This structured approach forms the basis of bowel control physiotherapy in Houston, Texas, that residents seek when conservative care matters. I also provide faecal incontinence rehab for clients looking for non-surgical rehabilitation.
Can Pelvic Floor Therapy Help Fecal Incontinence?
Yes. Clinical studies report meaningful improvement in 50 to 80 percent of patients who complete supervised pelvic floor rehabilitation. Outcomes improve when therapy addresses strength , coordination and diet together.
The pelvic floor therapy for fecal incontinence we offer in Memorial, TX, often improves urgency control and reduces accidents within weeks of structured practice. Bowel continence therapy in Bellaire, Texas, follows similar evidence-based principles.
Home Strategies That Support Therapy
Lifestyle adjustments support rehabilitation, though they do not replace evaluation.
- Increase soluble fiber to regulate stool consistency
- Limit caffeine if urgency worsens
- Maintain hydration
- Avoid chronic straining
- Track food triggers
- Know inflammatory foods and lifestyle
Diet influences stool form, which influences continence.
When to Seek Professional Evaluation
Seek evaluation if leakage persists, worsens, or disrupts daily life. Urgent neurological symptoms such as leg weakness or numbness in the lower pelvic region require immediate medical care.
Persistent urgency, staining, or accidents signal the need for a structured assessment.
Many individuals look for bowel dysfunction treatment in Spring Branch, TX, or bowel control physiotherapy in Houston, Texas, once symptoms interfere with work, travel, or intimacy. Others seek pelvic floor therapy for faecal incontinence in Memorial, TX, after childbirth or bowel surgery. Some pursue bowel continence therapy in Bellaire, Texas, when aging changes control.
My Approach at Beckham Physical Therapy and Wellness
I treat bowel incontinence through direct assessment and structured rehabilitation. I do not rely on generalized instruction. I evaluate strength, coordination, sensation, breathing mechanics, bowel habits and diet before designing a plan.
When childbirth contributes to symptoms, I address tissue recovery and muscle retraining. When aging reduces endurance, I build progressive strength and delay capacity. When constipation drives overflow leakage, I retrain bowel mechanics and eliminate strain patterns.
Individuals who begin bowel control physiotherapy in Houston, Texas, programs with me often notice early improvement in urgency control as coordination improves.
Some patients travel from surrounding communities. A person searching for pelvic floor therapy for fecal incontinence in Memorial TX often seeks specialized, hands-on evaluation rather than exercise handouts. Others looking into bowel continence therapy in Bellaire, Texas usually want measurable improvement and privacy in care. I treat both groups with the same clinical framework: assess precisely, retrain deliberately, measure progress.
Progress builds through repetition and correction. Control improves when muscles contract at the correct time and relax at the correct time.
Final Thoughts
Bowel incontinence affects millions. It reflects muscle coordination, nerve signaling, and stool consistency working out of sync. Structured rehabilitation restores alignment between these systems.
If bowel leakage disrupts life, structured pelvic floor rehabilitation offers evidence-based path toward improvement. Schedule a private consultation with me at
Beckham Physical Therapy and Wellness to begin restoring control and confidence.