Leaking When You Cough, Laugh, or Exercise? Understanding Stress Urinary Incontinence (SUI) and Your Treatment Options

Leaking urine when you cough, laugh, lift, or exercise often feels isolating. Many people reduce activity, avoid social settings, and carry spare clothing. Stress urinary incontinence affects millions of women and men across the United States. Clinical data show it accounts for nearly half of urinary incontinence cases in women. Men experience it most often after prostate surgery.
If you search for stress urinary leakage treatment in Memorial, Houston, Texas, you likely deal with this exact pattern. Leakage with movement signals a mechanical issue in pelvic support and coordination. It does not signal weakness of character or lack of effort. It signals a system that needs retraining.
I treat this condition every week in my practice. With focused pelvic floor rehabilitation, most people regain control and confidence.
What Is Stress Urinary Incontinence?
Stress urinary incontinence, often abbreviated SUI, describes involuntary urine leakage during activities that increase abdominal pressure. Coughing, sneezing, laughing, jumping, running, and lifting raise pressure inside the abdomen and bladder. When urethral closure pressure fails to match that increase, urine escapes.
This condition differs from urge incontinence. Urge incontinence involves a sudden, intense need to urinate followed by leakage. Mixed incontinence combines both patterns. Clear distinction matters because the treatment strategy depends on the mechanism.
People often ask, “Why do I leak when I cough or laugh?” Leakage occurs because pelvic floor muscles and connective tissue no longer stabilize the urethra effectively with increase in intra-abdominal pressure.
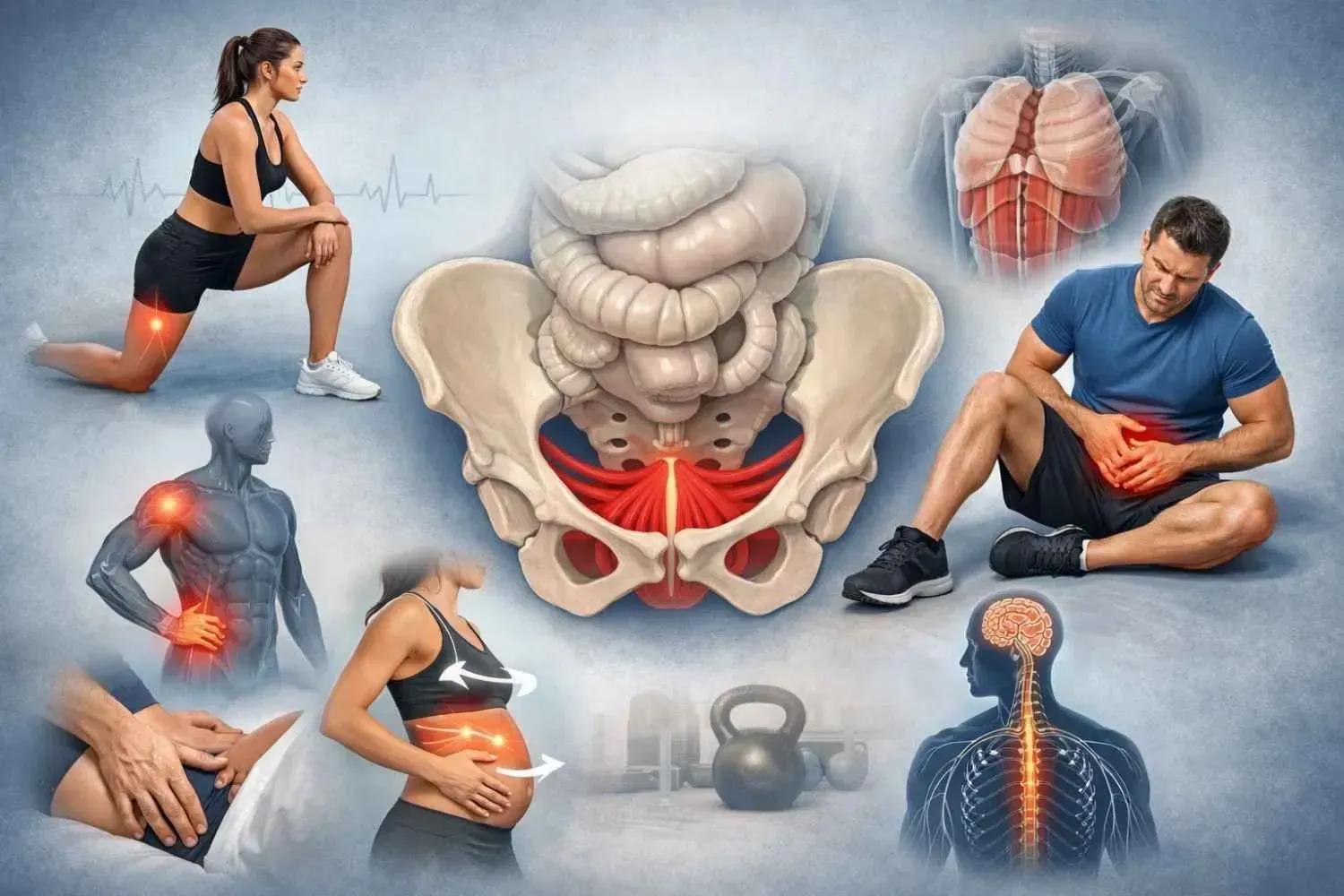
Why Leakage Happens: Mechanics Behind SUI
The bladder sits above the pelvic floor. The urethra runs from the bladder through the pelvic floor and rests behind the pubic bone. During a cough or jump, abdominal muscles contract, and intra-abdominal pressure rises sharply. Pelvic floor muscles must contract in coordination and create counterpressure. When they fail to respond with enough strength or timing, the potential for urine leakage occurs.
Research in pelvic health literature identifies two primary contributors:
- Pelvic floor muscle weakness or poor coordination
- Urethral sphincter insufficiency and connective tissue laxity
Pregnancy and vaginal delivery stretch pelvic tissue. Menopause alters collagen quality and tissue resilience. High body mass increases baseline abdominal pressure. Chronic coughing and constipation create repeated strain. Prostate surgery affects urethral sphincter function in men.
Athletes face unique risks. High impact activity such as running, gymnastics, or CrossFit produce repeated spikes in intra-abdominal pressure. Many athletic adults seek urinary leakage with exercise treatment in Houston, TX, after symptoms disrupt training.
Who Faces Higher Risk?
Women
- Pregnancy and vaginal delivery
- Baby's weight is over nine pounds
- Instrument-assisted delivery
- Perimenopause and menopause
- Pelvic organ prolapse
- Overweight
Men
- Prostatectomy
- Other pelvic surgery
- Overweight
Both
- Chronic constipation
- Chronic cough
- High BMI
- Repetitive heavy lifting
- High-impact sport
Postpartum women often assume leakage represents a normal stage of recovery. Research shows pelvic floor muscle training significantly reduces symptoms when started early.
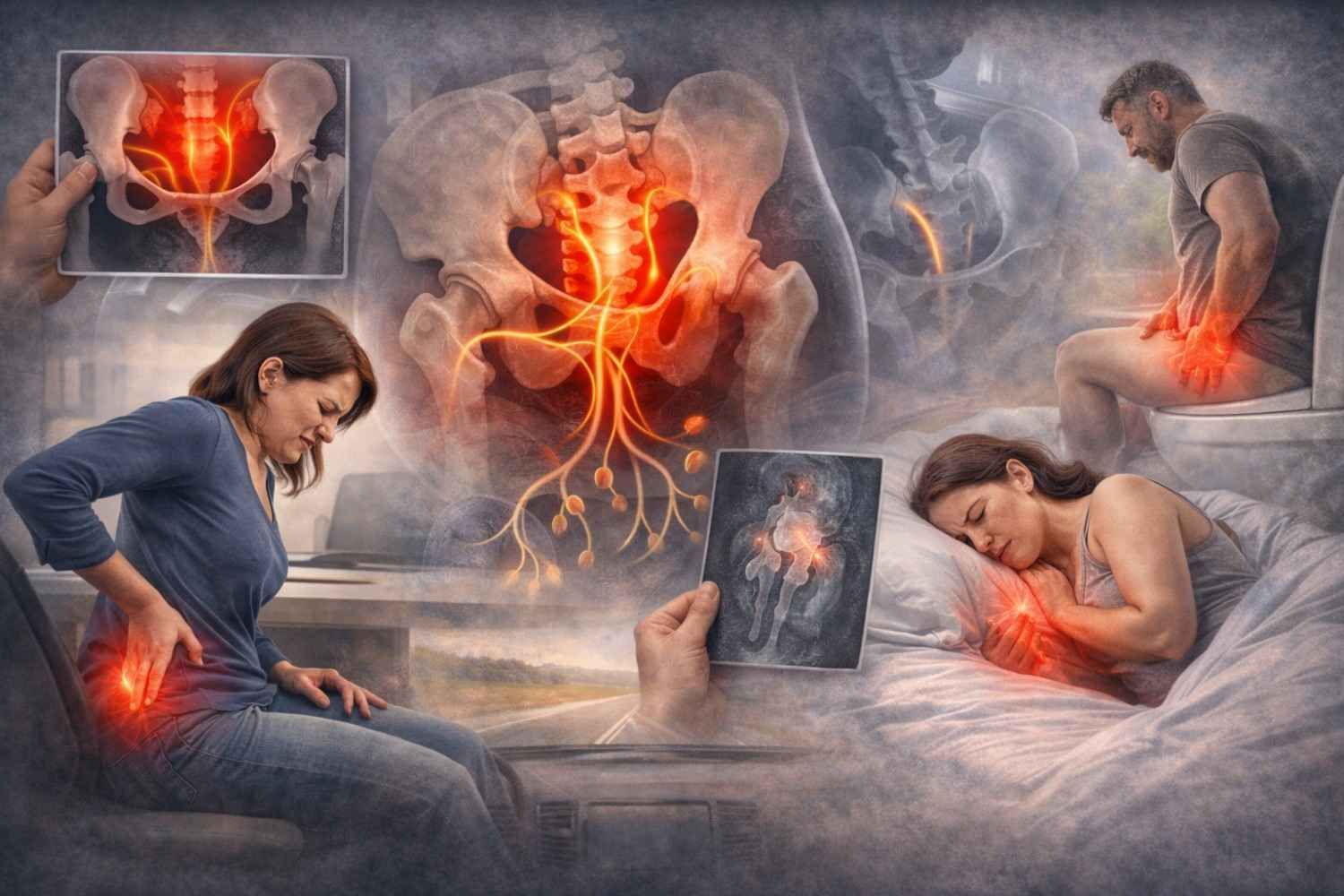
Symptoms That Affect Daily Life
Stress urinary incontinence rarely stops at a few drops. People report:
- Leakage during exercise or lifting
- Leakage during laughter or sudden movement
- Wearing pads for security
- Avoiding social or athletic events
- Fear of visible wetness
If you ask, “Do I have stress urinary incontinence?” and leakage aligns with movement rather than urgency, SUI likely plays a role.
How I Diagnose Stress Urinary Incontinence
At my practice, Beckham Physical Therapy and Wellness, I begin with a detailed history. I review bladder habits, bowel patterns, activity level, and surgical history. I assess posture, breathing mechanics, hip strength, and abdominal coordination.
The pelvic floor muscle exam evaluates tone, strength, endurance, and timing. Many people contract their muscles or hold their breath during an effort. Individuals searching for a stress urinary incontinence clinic in Bunker Hill Villages, TX, or a stress urinary incontinence specialist in Memorial, TX, often want clarity. Clear diagnosis directs effective care.
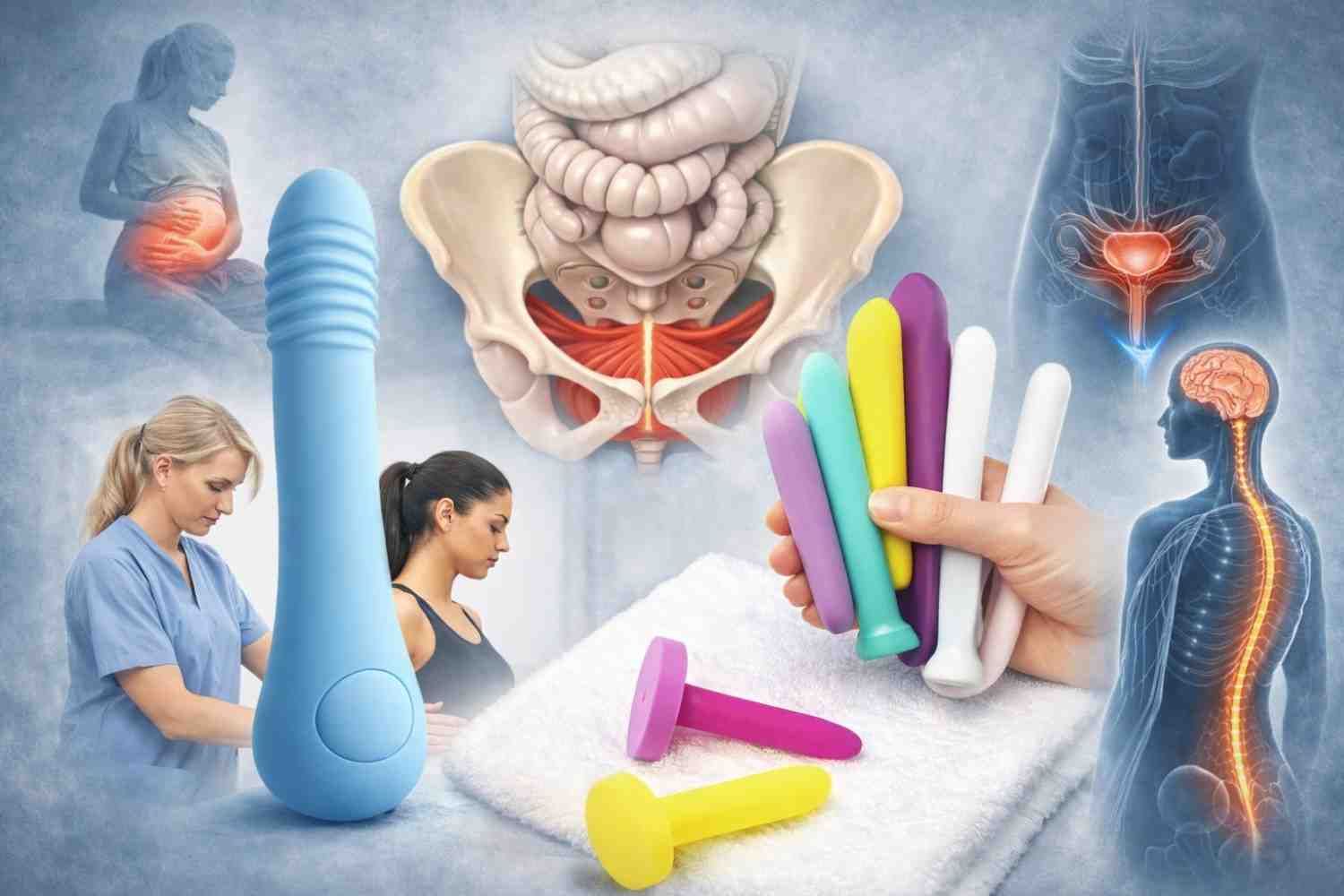
Treatment Options: Evidence-Based Approach
Pelvic Floor Rehabilitation: First Line Strategy
Clinical guidelines from urology and gynecology associations recommend pelvic floor muscle training as first-line management for stress urinary incontinence. Supervised training improves outcomes compared to unsupervised exercises.
Pelvic floor rehab for stress incontinence in Houston, Texas, focuses on:
- Targeted strength training
- Coordination and timing drills
- Breath control during exertion
- Functional integration into lifting, running, and coughing
- Manual therapy to address tension or scar tissue
- Core and hip support
Kegels alone often fail because people either contract incorrectly or isolate muscles without functional integration. Effective therapy trains the pelvic floor to respond automatically before pressure rises.
Patients seeking stress incontinence pelvic floor physiotherapy in Bellaire, TX, benefit from individualized programming rather than generic instruction sheets.
Behavioral and Lifestyle Support
Therapy also addresses contributing factors:
- Improve fiber intake to reduce straining
- Optimize fluid timing
- Reduce excessive caffeine if it irritates the bladder.
- Address chronic cough
- Manage body weight
Lifestyle modification supports muscle recovery. Muscle training drives primary change.
Surgical and Device Options
Sling procedures, urethral bulking agents, and pessaries provide structural support in selected cases. Surgery serves individuals with severe sphincter deficiency or persistent symptoms after conservative care. Many people improve significantly without operative intervention.
I discuss these options when appropriate and coordinate with physicians if symptoms fail to respond to rehabilitation.
What Pelvic Floor Therapy Looks Like With Me
I work one-on-one with each client. Sessions focus on precise motor control and measurable progress. I teach you how to contract the pelvic floor before coughing or lifting. We practice coordination during real-world tasks.
Treatment often includes:
- Internal muscle assessment
- Strength progression
- Endurance training
- Movement retraining
- Education on bladder habits
Clients seeking stress urinary leakage treatment in Memorial, Houston, Texas, often notice improvement within six to eight weeks when they practice consistently. Post-prostate surgery cases may require a longer timeline, often three to six months.
How Long Does Recovery Take?
Research on pelvic floor muscle training shows a meaningful reduction in leakage within twelve weeks for many individuals.Many of my clients find reduction in 6 to 8 weeks. Adherence influences outcome. Muscle hypertrophy and neuromuscular adaptation require repetition and progression.
Athletes often regain control as coordination improves. Postpartum women frequently see a change once muscle activation normalizes. Men recovering from prostate surgery experience gradual improvement as sphincter strength returns.
When to Seek Help
Leakage during activity does not resolve on its own in many cases. Early evaluation prevents compensation patterns and activity avoidance. If leakage interferes with exercise, work, or confidence, a professional assessment offers direction.
Individuals searching for pelvic floor rehab for stress incontinence or urinary leakage with exercise treatment in Houston, TX, often reach out after months of frustration. Earlier intervention shortens recovery.
Regain Control and Confidence
Stress urinary incontinence affects the body and identity. It alters how you move, socialize, and train. Evidence supports pelvic floor rehabilitation as effective first-line care. Precise assessment and individualized training restore urethral support and timing.
At Beckham Physical Therapy and Wellness, I serve clients across Memorial, Bellaire, Bunker Hill Villages, and the greater Houston area. If you seek a stress urinary incontinence (SUI) specialist in Memorial, TX, schedule a consultation. Together, we identify the cause, design a plan, and restore control. Contact me today.